BLog & News
We will continously blog on our own and others results on cord clamping, as well as other news related to the subject, such as umbilical cord milking and resuscitation.
Latest posts from the blog
When a baby is born, it's an exciting moment for all involved. But there are still some important decisions to be made in the moments after birth – one of which is when to clamp and cut the umbilical cord. While most parents may feel inclined to do this immediately following delivery, experts suggest that waiting a few minutes has many potential benefits for both mother and child. In this article, we'll discuss three of these advantages associated with delaying umbilical cord clamping.
As soon as a baby enters the world, they must now learn how to survive outside the womb on their own. During this time, having access to blood from the placenta can help them make this transition easier. This vital resource includes essential nutrients like iron along with oxygen-rich red blood cells – giving newborns a much needed boost at such a fragile stage in life. Clamping too quickly can mean depriving your little one of these critical elements right when they require them most.
Finally, delayed cord clamping also offers certain health benefits for mothers as well. When babies receive more placental blood before cutting ties with mom, research suggests it might reduce risk factors associated with postpartum hemorrhage – something no new parent wants to experience! So if you're expecting or already have welcomed your bundle of joy into the family, consider taking extra time before severing that special bond between parent and child via the umbilical cord!
Benefits Of Delayed Cord Clamping
Clamping the umbilical cord is a significant step in childbirth and can have long-term impacts on both mother and baby. Delayed cord clamping has many benefits that should not be overlooked; here we examine three reasons to wait before clamping the umbilical cord.
Firstly, delayed cord clamping helps promote better iron levels in newborns. By waiting for at least 30 seconds after birth to cut the cord, babies can receive more oxygenated blood from mom's placenta, which boosts their iron stores significantly. This allows infants to develop higher hemoglobin levels in their bodies, reducing the risk of anemia down the road into childhood.
Secondly, delayed cord clamping encourages healthy growth in newborns by providing additional nutrients through placental transfusion. Studies show that these unique transfers can increase birth weight and ward off potential problems such as hypoglycemia, bradycardia and respiratory distress syndrome. Allowing time for further placental transfusions may also lead to improved breastfeeding rates since it gives babies access to colostrum – mom's special milk full of antibodies - right away.
Finally, delaying cord clamping allows for longer bonding between mom and baby immediately following birth. Without rushing this process with early clamping, mothers get a chance to experience skin-to-skin contact with their infant shortly after delivery while still connected via the umbilical cord. This provides ample opportunity for moms and babies alike to share meaningful moments together even amidst all the chaos of labor and delivery!
Delaying or avoiding immediate cutting of the umbilical cord comes with several important advantages for parents looking for ways to nurture their little ones throughout pregnancy and beyond. With these numerous benefits associated with delayed cord clamping come certain risks which will be discussed next...
Risks Of Early Cord Clamping
When it comes to clamping the umbilical cord, timing is everything. A newborn’s health and wellbeing depend on when this important step occurs. Early clamping carries its own risks, making delayed clamping a far better option for both mother and baby.
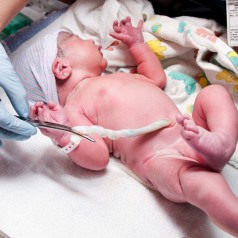
The image of a pair of scissors snipping through the lifeline that connects mother and child can be jarring; however, understanding why early cord clamping must be avoided is crucial. The possible consequences include:
- Impaired iron stores leading to anemia
- Disrupted thermoregulation (body temperature control)
- Difficulty transitioning from intrauterine to extra uterine life
These potential issues run the gamut from mild to severe in their effects – ranging anywhere from short-term fatigue or jaundice to long-term neurodevelopmental impairments. Additionally, as research continues into other areas such as immune system development, more complications may become apparent with early cord clamping.
Given all these considerations, delaying cord clamping until after birth offers many advantages without any known disadvantages. It's essential for parents to have access to accurate information regarding safe delay practices so they can make informed decisions about their care during labor and delivery.
How To Safely Delay Clamping The Umbilical Cord
The umbilical cord is a vital lifeline between mother and child, yet many parents opt to have the umbilical cord clamped immediately after birth. Ironically, this seemingly innocuous action could actually be harmful – so how can you safely delay clamping it?
It’s important not to rush into clamping the umbilical cord. It's best practice that both baby and mother benefit from delayed cord clamping by allowing time for placental transfusion of oxygen-rich blood as well as essential nutrients and iron stores. In addition, waiting a few minutes allows gravity to reduce the pressure in the placenta, which helps reduce bleeding at delivery.
To ensure a safe transition for your newborn, keep him or her warm during skin-to-skin contact with mom (known as “kangaroo care”). This will help maintain their temperature while stabilizing heart rate and respiratory rates. During this time, an experienced midwife should monitor both mother and baby closely, including checking blood pressures every five minutes until stabilized. This period usually lasts about fifteen minutes before considering cutting the umbilical cord if medically necessary.
In order to minimize any risks associated with early clamping of the umbilical cord, delaying for even three more minutes beyond when baby has been delivered gives them valuable extra time on the life-giving connection they shared throughout pregnancy — one last chance to receive what they need before entering into this new world!
Conclusion
In conclusion, waiting to clamp the umbilical cord is beneficial for both the baby and mother. Delayed cord clamping increases a newborn's iron stores and red blood cells, which can help prevent anemia in infancy. It also reduces risks of preterm infants developing intraventricular hemorrhage or necrotizing enterocolitis later on. Additionally, it helps ensure that a newborn receives all the placental transfusions they need while reducing their risk of needing a blood transfusion.
Research shows that delaying cord clamping by just one minute can increase hemoglobin levels in term babies by 10%. So even if you're pressed for time after delivery, taking a minute to wait before cutting the umbilical cord could be life-changing for your little one!
Research
Latest posts on NEW research
The timing of umbilical cord clamping has been a topic of considerable debate in the medical community, particularly concerning preterm infants. A recent study aimed to shed light on this issue and understand how early or delayed cord clamping affects the health outcomes of these vulnerable newborns.
Methodology:
Researchers conducted a study involving 96 pregnant women eagerly awaiting the arrival of their babies. The participants were randomly assigned to one of two groups - early cord clamping (ECC) or delayed cord clamping (DCC). The researchers closely monitored hematological and cardiac changes in the preterm infants, focusing on gestational periods between 24 and 34 weeks, and evaluated the stability of key blood parameters within the first week after birth.
Key Findings:
The study revealed interesting insights into the impact of cord clamping timing. Infants in the DCC group showed higher levels of hemoglobin and hematocrit upon admission, indicating improved oxygen-carrying capacity compared to those in the ECC group. Similarly, by the seventh day of life, the DCC group maintained higher hemoglobin and hematocrit levels, suggesting continued hematological advantages.
However, it should be noted that the DCC group also had a slightly higher incidence of phototherapy usage to treat jaundice compared to the ECC group.
Cardiac parameters and maternal blood tests did not differ significantly between the two groups.
Conclusion:
The study suggests that delayed cord clamping may have certain benefits for preterm infants in terms of hematological outcomes, as evidenced by higher hemoglobin and hematocrit levels. However, it is important to consider that other factors, such as a slightly increased need for phototherapy, should be taken into account.
This study adds valuable insights to the ongoing discussion regarding the optimal timing for cord clamping in preterm births. Further research is warranted to better understand the long-term implications and overall health outcomes associated with cord clamping practices.
Reference: García, C., Prieto, M.T., Escudero, F., Bosh-Giménez, V., Quesada, L., Lewanczyk, M., Pertegal, M., Delgado, J.L., Blanco-Carnero, J.E., De Paco Matallana, C., 2023. The impact of early versus delayed cord clamping on hematological and cardiovascular changes in preterm newborns between 24 and 34 weeks’ gestation: a randomized clinical trial. Archives of Gynecology and Obstetrics.. https://doi.org/10.1007/s00404-023-07119-0
Understanding the Dynamics of Umbilical Cord Circulation and Placental Transfusion: Debunking Common
Newsletter
WHAt Do Others Write

Laddar innehåll...
cord clamping newborn
-
A Study on the Effect of Umbilical Cord Milking Along With Delayed Cord Clamping on Hematological Parameters in Comparison to Delayed Cord Clamping Alone in Moderate-to-Late Preterm Newborns
Cureus. 2024 Sep 12;16(9):e69256. doi: 10.7759/cureus.69256. eCollection 2024 Sep.ABSTRACTBackground Anemia, particularly iron deficiency anemia (IDA), is a global public health issue with serious implications for infant cognitive and developmental outcomes. Preterm infants are especially vulnerable to IDA due to reduced placental blood transfer at birth. Delayed cord clamping (DCC) and umbilical cord milking (UCM) are interventions aimed at enhancing this blood transfer, thereby improving neonatal iron status. While DCC allows passive blood transfer by delaying cord clamping, UCM actively expedites the process. However, there remains a lack of consensus on the comparative benefits of these methods, particularly in preterm infants. This study aims to clarify the efficacy of UCM combined with DCC versus DCC alone in improving hematological outcomes in moderate-to-late preterm newborns. Methodology This comparative study was conducted at Maharaja Agrasen Medical College, Agroha, Hisar, Haryana, over a 12-month period. The study included 200 moderate-to-late preterm infants (32-36+6 weeks of gestation), divided into two groups: Group A (DCC alone) and Group B (DCC combined with UCM). The study aimed to compare the effects of these two interventions on hematological outcomes. Data were collected on baseline characteristics, birth weight, hemoglobin (Hb) levels at birth and at six weeks, serum ferritin levels at six weeks, and any complications. Statistical analyses included independent t-tests for continuous variables and chi-squared tests for categorical variables to assess the differences between the two groups. Results There were no significant differences in the baseline characteristics, birth weight, or clamping time between the two groups. Mean Hb levels at birth were 15.46 g/dL in the DCC group and 15.72 g/dL in the DCC+UCM group (p = 0.429). At six weeks, the mean Hb levels were 13.10 g/dL for the DCC and 13.24 g/dL for the DCC+UCM (p = 0.541). Serum ferritin levels at six weeks were 239.26 ng/mL for the DCC and 258.06 ng/mL for DCC+UCM (p = 0.146). Complications were similar between the groups, with no significant differences in the rates of intraventricular hemorrhage (IVH), jaundice, or polycythemia. Conclusion In this study, the combination of UCM with DCC did not show significant differences in hematological outcomes compared to DCC alone in moderate-to-late preterm infants. Both interventions demonstrated similar results for hemoglobin and ferritin levels, and there were no notable differences in adverse outcomes. Further research with larger sample sizes and longer follow-ups is necessary to better understand the potential benefits of UCM in preterm neonates.PMID:39403649 | PMC:PMC11472205 | DOI:10.7759/cureus.69256… -
Oxygenation associated with cord management strategies among preterm infants
J Perinatol. 2024 Oct 11. doi: 10.1038/s41372-024-02127-7. Online ahead of print.ABSTRACTOBJECTIVE: Compare changes in SpO2 and FiO2 post-birth among preterm infants after delayed cord clamping (DCC), umbilical cord milking (UCM) or early cord clamping (ECC).STUDY DESIGN: Retrospective study of infants <32 weeks gestation born between 2014 and 2021. ECC was clamping 0-59 s, DCC was clamping ≥60 s after delivery, UCM defined as milking the intact umbilical cord several times before clamping.RESULTS: Of 463 infants; 257 received DCC, 168 received UCM, 38 received ECC. UCM infants had higher median SpO2 values at 4-(79% UCM vs 69% DCC, p = 0.027) and 5-(85% UCM vs 80% DCC, p = 0.023) minutes after-birth compared to DCC. DCC and UCM infants required lower FiO2 levels in the first 5-minutes compared to ECC infants (DCC 0.38 ± 0.17, UCM 0.40 ± 0.20 vs ECC 0.51 ± 0.27, p's <0.001).CONCLUSION: The proportion of infants achieving SpO2 ≥ 80% by 5 min was similar in all groups, FiO2 needed to achieve this goal was higher in ECC infants.PMID:39394453 | DOI:10.1038/s41372-024-02127-7… -
Revolutionizing Neonatal Care: A Comprehensive Review of Intact Cord Resuscitation in Newborns
Cureus. 2024 Sep 8;16(9):e68924. doi: 10.7759/cureus.68924. eCollection 2024 Sep.ABSTRACTNeonatal resuscitation is a critical procedure aimed at ensuring the successful transition of newborns from intrauterine to extrauterine life. Traditionally, this involves immediate clamping and cutting of the umbilical cord, but recent advances have introduced intact cord resuscitation (ICR) as an alternative approach. This review aims to comprehensively analyze ICR, exploring its evolution, scientific basis, and clinical evidence. It seeks to evaluate the benefits and challenges associated with ICR and assess its impact on neonatal outcomes compared to traditional practices. A thorough review of the literature was conducted, including historical perspectives on neonatal resuscitation, the physiological rationale behind ICR, and critical clinical studies and trials. Current guidelines and recommendations were also examined, along with technological advancements and practical implementation issues. Evidence indicates that ICR offers significant benefits, including improved blood volume, better cardiovascular stability, and reduced risk of anemia in newborns. Comparative studies suggest that ICR can enhance neonatal outcomes and support a smoother transition to extrauterine life. Despite these benefits, challenges related to implementation and adherence to new practices persist. ICR represents a promising advancement in neonatal care, potentially improving newborns' health outcomes. Continued research and refinement of guidelines are necessary to fully integrate ICR into standard practice and address existing implementation challenges. This review highlights the need for ongoing evaluation and adaptation of resuscitation practices to optimize neonatal health and care.PMID:39381456 | PMC:PMC11459599 | DOI:10.7759/cureus.68924… -
Evaluating the efficacy of endotracheal and intranasal epinephrine administration in severely asphyxic bradycardic newborn lambs: a randomised preclinical study
Arch Dis Child Fetal Neonatal Ed. 2024 Sep 4:fetalneonatal-2024-327348. doi: 10.1136/archdischild-2024-327348. Online ahead of print.ABSTRACTOBJECTIVE: Intravenous epinephrine administration is preferred during neonatal resuscitation, but may not always be rapidly administered due to lack of equipment or trained staff. We aimed to compare the time to return of spontaneous circulation (ROSC) and post-ROSC haemodynamics between intravenous, endotracheal (ET) and intranasal (IN) epinephrine in severely asphyxic, bradycardic newborn lambs.METHODS: After instrumentation, severe asphyxia (heart rate <60 bpm, blood pressure ~10 mm Hg) was induced by clamping the cord in near-term lambs. Resuscitation was initiated with ventilation followed by chest compressions. Lambs were randomly assigned to receive intravenous (0.02 mg/kg), ET (0.1 mg/kg) or IN (0.1 mg/kg) epinephrine. If ROSC was not achieved after three allocated treatment doses, rescue intravenous epinephrine was administered. After ROSC, lambs were ventilated for 60 min.RESULTS: ROSC in response to allocated treatment occurred in 8/8 (100%) intravenous lambs, 4/7 (57%) ET lambs and 5/7 (71%) IN lambs. Mean (SD) time to ROSC was 173 (32) seconds in the intravenous group, 360 (211) seconds in the ET group and 401 (175) seconds in the IN group (p<0.05 intravenous vs IN). Blood pressure and cerebral oxygen delivery were highest in the intravenous group immediately post-ROSC (p<0.05), whereas the ET group sustained the highest blood pressure over the 60-min observation (p<0.05).CONCLUSION: Our study supports neonatal resuscitation guidelines, highlighting intravenous administration as the most effective route for epinephrine. ET and IN epinephrine should only be considered when intravenous access is delayed or not feasible.PMID:39237256 | DOI:10.1136/archdischild-2024-327348… -
Umbilical cord management in newborn resuscitation: a systematic review and meta-analysis
Pediatr Res. 2024 Sep 2. doi: 10.1038/s41390-024-03496-7. Online ahead of print.ABSTRACTBACKGROUND: Evidence supporting the benefits of delayed cord clamping is increasing; however, there is no clear recommendation on cord management during newborn resuscitation. This study aimed to investigate the effects of resuscitation initiated with an intact umbilical cord, hypothesizing it is a safe stabilization procedure that improves neonatal outcomes.METHODS: Systematic search was conducted in MEDLINE, Embase, CENTRAL, and Web of Science from inception to March 1, 2024. Eligible articles compared neonatal outcomes in newborns receiving initial stabilization steps before and after cord clamping.RESULTS: Twelve studies met our inclusion criteria, with six RCTs included in the quantitative analysis. No statistically significant differences were found in delivery room parameters, in-hospital mortality, or neonatal outcomes between the examined groups. However, intact cord resuscitation group showed higher SpO2 at 5 min after birth compared to cord clamping prior to resuscitation group (MD 6.67%, 95% CI [-1.16%, 14.50%]). There were no significant differences in early complications of prematurity (NEC ≥ stage 2: RR 2.05, 95% CI [0.34, 12.30], IVH: RR 1.25, 95% CI [0.77, 2.00]).CONCLUSION: Intact cord management during resuscitation appears to be a safe intervention; its effect on early complications of prematurity remains unclear. Further high-quality RCTs with larger patient numbers are urgently needed.IMPACT: Initiating resuscitation with an intact umbilical cord appears to be a safe intervention for newborns. No statistically significant differences were found in delivery room parameters, in-hospital mortality, and neonatal outcomes between the examined groups. The utilization of specialized resuscitation trolleys appears to be promising to reduce the risk of intraventricular hemorrhage in preterm infants. Further high-quality RCTs with larger sample sizes are urgently needed to refine recommendations.PMID:39223253 | DOI:10.1038/s41390-024-03496-7… -
Detection of time of birth and cord clamping using thermal video in the delivery room
Front Pediatr. 2024 Aug 14;12:1342415. doi: 10.3389/fped.2024.1342415. eCollection 2024.ABSTRACTINTRODUCTION: Newborn resuscitation algorithms emphasize that resuscitation is time-critical, and all algorithm steps are related to the time of birth. Infrared thermal video has the potential to capture events in the delivery room, such as birth, cord clamping, and resuscitative interventions, while upholding the privacy of patients and healthcare providers.OBJECTIVES: The objectives of this concept study were to (i) investigate the technical feasibility of using thermal video in the delivery room to detect birth and cord clamping, and (ii) evaluate the accuracy of manual real-time registrations of the time of birth and cord clamping by comparing it with the accuracy of registrations abstracted from thermal videos.METHODS: An observational study with data collected at Stavanger University Hospital, Norway, from September 2022 to August 2023. The time of birth and cord clamping were manually registered on a portable tablet by healthcare providers. Thermal cameras were placed in the delivery rooms and operating theatre to capture births. Videos were retrospectively reviewed to determine the time of birth and cord clamping.RESULTS: Participation consent was obtained from 306 mothers, of which 195 births occurred in delivery rooms or an operating theatre with a thermal camera installed. We excluded 12 videos in which no births occurred. Births were detectable in all 183 (100%) thermal videos evaluated. There was a median (quartiles) of 1.8 (0.7, 5.4) s deviation in the manual registrations of the times of births relative to those abstracted from thermal videos. Cord clamping was detectable in 173 of the 183 (95%) thermal videos, with a median of 18.3 (3.3, 108) s deviation in the manual registrations of the times of cord clampings relative to those abstracted from thermal videos.CONCLUSION: Recognizing the time of birth and cord clamping from thermal videos is technically feasible and provides a method for determining when resuscitative events occur.PMID:39205665 | PMC:PMC11349661 | DOI:10.3389/fped.2024.1342415… -
Physiological-Based Cord Clamping: When the Baby Is Ready for Clamping
Neonatology. 2024;121(5):547-552. doi: 10.1159/000540667. Epub 2024 Aug 28.ABSTRACTBACKGROUND: The timing of cord clamping has become a focal point for neonatal caregivers due to the promising outcomes associated with delayed cord clamping, which is a simple and cost-effective method to enhance the survival and well-being of preterm infants. While initially the rationale behind delaying clamping was to facilitate increased placental transfusion, research has unveiled additional hemodynamic benefits.SUMMARY: Experimental studies have demonstrated improved circulatory transition when clamping is postponed until the lungs are adequately aerated. This suggests that infants requiring assistance during the transition phase may benefit from stabilization while still attached to the cord. The Aeration, Breathing, and then Clamping (ABC) project aimed to translate these experimental findings into clinical practice.KEY MESSAGE: In this review, we will discuss the insights gained and lessons learned from the project's implementation.PMID:39197438 | PMC:PMC11446291 | DOI:10.1159/000540667… -
Maternal antibiotic prophylaxis during cesarean section has a limited impact on the infant gut microbiome
Cell Host Microbe. 2024 Aug 14;32(8):1444-1454.e6. doi: 10.1016/j.chom.2024.07.010.ABSTRACTPregnant women undergoing a cesarean section (CS) typically receive antibiotics prior to skin incision to prevent infections. To investigate if the timing of antibiotics influences the infant gut microbiome, we conducted a randomized controlled trial (NCT06030713) in women delivering via a scheduled CS who received antibiotics either before skin incision or after umbilical cord clamping. We performed a longitudinal analysis on 172 samples from 28 infants at 8 post-birth time points and a cross-sectional analysis at 1 month in 79 infants from 3 cohorts. Although no significant associations with bacterial composition, metabolic pathways, short-chain fatty acids, and bile acids were found, we observed subtle differences between the groups at the bacterial strain level and in the load of antibiotic resistance genes. Rather, feeding mode was a predominant and defining factor impacting infant microbial composition. In conclusion, antibiotic administration during CS has only limited effects on the early-life gut microbiome.PMID:39146801 | PMC:PMC11335186 | DOI:10.1016/j.chom.2024.07.010… -
The application of cut-umbilical cord milking in term cesarean deliveries for preventing anemia and iron deficiency of newborns
Zhonghua Yi Xue Za Zhi. 2024 Aug 20;104(32):3042-3049. doi: 10.3760/cma.j.cn112137-20240621-01378.ABSTRACTObjective: To anlysis the efficacy and safety of cut-umbilical cord milking (C-UCM) compared with immediate cord clamping in preventing anemia and iron deficiency among term cesarean-delivered newborns. Methods: A total of 485 pregnant women planning to deliver by cesarean section were recruited in this randomized controlled trial in Hunan Maternal and Child Health Hospital and Liuyang Maternal and Child Health Care Hospital from July 2016 to April 2019. A block randomization was conducted to evenly allocate them to the controlled group and the C-UCM group. In the controlled group, the cord was clamped within 30 seconds as routine. In the C-UCM group, the cord was first clamped at 25 cm from the newborn's navel, and then the blood in the cord was gently squeezed into the newborn's body until the cord became white and shriveled. The cord was clamped twice at 2-3 cm from the newborn's navel subsequently. Neonatal jaundice, hyperbilirubinemia and polycythemia were monitored before discharge. After the newborns discharged, their hemoglobin, red blood cell count, hematocrit (at the age of 1, 6 and 12 months) and serum ferritin (at the age of 6 and 12 months) were followed up; body length and weight were measured; and information about their feeding and iron supplementation were collected (at the age of 1, 6, 12 and 18 months). The two groups were compared by t test, Mann-Whitney U test, χ² test, or Fisher exact probability method. The hospital was set as a random item, and the mixed effects regression model was used to evaluate the effect of C-UCM on relevant indicators of cesarean-delivered newborns. Results: There were 244 women in the C-UCM group with an average age of (31.9±4.4) years, and 241 in the control group with an average age of (31.8±4.2) years (P>0.05). There was no statistically significant difference between the C-UCM group and the control group at 1, 6 and 12 months of age in hemoglobin [(123.6±14.5) vs (122.2±14.5) g/L, (115.3±9.4) vs (114.1±8.5) g/L, (115.6±9.6) vs (116.1±12.6) g/L] or anemia incidence rate [15.2% (17/112) vs 18.4% (19/103), 22.7% (34/150) vs 26.8% (44/164), 22.3% (25/112) vs 19.5% (22/113)] (all P>0.05). There was no statistically significant difference between the two groups at 6 and 12 months of age in serum ferritin [M (Q1, Q3), 39.9 (24.9, 61.8) vs 43.6 (25.2, 100.9) μg/L, 40.3 (25.4, 259.2) vs 40.3 (26.4, 167.6) μg/L)] or iron deficiency incidence rate [6.1% (5/82) vs 4.2% (3/72), 6.7% (5/75) vs 3.8% (3/80)] (all P>0.05). There were also no significant difference between the two groups in other indicators, such as the Z-score of weight-for-length, the incidence of neonatal jaundice, and the incidence of neonatal hyperbilirubinemia (all P>0.05). After adjusting for the relevant covariates, there were still no significant effects of C-UCM on these outcomes above. Conclusions: Compared to immediate cord clamping, the intervention of gently squeezing 25 cm of the cord does not significantly reduce the risk of anemia or iron deficiency in term cesarean-delivered newborns, nor does it have a significant impact on infant growth and development. Yet this intervention does not increase the risk of jaundice or hyperbilirubinemia in newborns as well.PMID:39143772 | DOI:10.3760/cma.j.cn112137-20240621-01378… -
How to improve newborn outcomes in 60 s-delay clamping the umbilical cord
BMC Pregnancy Childbirth. 2024 Aug 14;24(1):534. doi: 10.1186/s12884-024-06467-2.ABSTRACTDeferred umbilical cord clamping (DCC) has been employed with wide variation in the United States over the last few decades. This practice has the potential to improve infant health and outcomes at the population health level. Education campaigns and policy interventions can promote DCC use in a safe manner.PMID:39143565 | PMC:PMC11323698 | DOI:10.1186/s12884-024-06467-2… -
Delaying cord clamping for more than 1 minute after vaginal deliveries appeared to result in smoother cardiocirculatory transition
Acta Paediatr. 2024 Nov;113(11):2411-2413. doi: 10.1111/apa.17373. Epub 2024 Aug 5.NO ABSTRACTPMID:39101781 | DOI:10.1111/apa.17373… -
Early or delayed cord clamping during transition of term newborns: does it make any difference in cerebral tissue oxygenation?
Ital J Pediatr. 2024 Jul 29;50(1):133. doi: 10.1186/s13052-024-01707-9.ABSTRACTBACKGROUND: According to the World Health Organization's recommendation, delayed cord clamping in term newborns can have various benefits. Cochrane metaanalyses reported no differences for mortality and early neonatal morbidity although a limited number of studies investigated long-term neurodevelopmental outcomes. The aim of our study is to compare the postnatal cerebral tissue oxygenation values in babies with early versus delayed cord clamping born after elective cesarean section.METHODS: In this study, a total of 80 term newborns delivered by elective cesarean section were included. Infants were randomly grouped as early (clamped within 15 s, n:40) and delayed cord clamping (at the 60th second, n:40) groups. Peripheral arterial oxygen saturation (SpO2) and heart rate were measured by pulse oximetry while regional oxygen saturation of the brain (rSO2) was measured with near-infrared spectrometer. Fractional tissue oxygen extraction (FTOE) was calculated for every minute between the 3rd and 15th minute after birth. (FTOE = pulse oximetry value-rSO2/pulse oximetry value). The measurements were compared for both groups.RESULTS: The demographical characteristics, SpO2 levels (except postnatal 6th, 8th, and 14th minutes favoring DCC p < 0.05), heart rates and umbilical cord blood gas values were not significantly different between the groups (p > 0.05). rSO2 values were significantly higher while FTOE values were significantly lower for every minute between the 3rd and 15th minutes after birth in the delayed cord clamping group (p < 0.05).CONCLUSION: Our study revealed a significant increase in cerebral rsO2 values and a decrease in FTOE values in the delayed cord clamping (DCC) group, indicating a positive impact on cerebral oxygenation and hemodynamics. Furthermore, the DCC group exhibited a higher proportion of infants with cerebral rSO2 levels above the 90th percentile. This higher proportion, along with a lower of those with such parameter below the 10th percentile, suggest that DCC may lead to the targeted/optimal cerebral oxygenetaion of these babies. As a result, we recommend measuring cerebral oxygenation, in addition to peripheral SpO2, for infants experiencing perinatal hypoxia and receiving supplemental oxygen.PMID:39075594 | PMC:PMC11288115 | DOI:10.1186/s13052-024-01707-9… -
Extended period of ventilation before umbilical cord clamping at birth: A study that mis-interprets and mis-represents the physiology
J Physiol. 2024 Sep;602(17):4327-4328. doi: 10.1113/JP286866. Epub 2024 Jul 15.NO ABSTRACTPMID:39008340 | DOI:10.1113/JP286866… -
Safety of different cord clamping strategies in the early postnatal period
Early Hum Dev. 2024 Aug;195:106075. doi: 10.1016/j.earlhumdev.2024.106075. Epub 2024 Jul 10.ABSTRACTBACKGROUND: This study aimed to evaluate the effect of ICC (cord clamping within the first 15 s), DCC (delayed cord clamping at 60 s), and cut-UCM (cut-umbilical cord milking, cord clamping within the first 15 s) groups on oxygen saturation (SpO2), heart rate (HR), and perfusion index (PI) up to 10 min after birth in newborn infants.METHODS: We conducted this randomized clinical trial in the delivery unit of a University Hospital with 189 infants born between 35 and 42 weeks of gestation. Participants were randomly assigned to one of three groups: ICC, DCC, and cut-UCM. The primary outcomes measured were SpO2, HR, and PI at the 1st, 3rd, 5th, and 10th minutes after birth. We utilized ANOVA and Bayesian calculations in this study.RESULTS: There was no difference between the ICC, DCC, and cut-UCM groups in SpO2, HR, and PI values at the 1st, 3rd, 5th, and 10th minutes of life, which did not significantly alter between the three groups in one-way ANOVA. Bayesian repeated-measure ANOVA calculations showed that SpO2 and heart rate results at the 1st, 3rd, 5th, and 10th minutes did not differ between ICC, DCC, and cut-UCM techniques with strong evidence. At the 3rd minute, PI was slightly higher in the DCC and cut-UCM groups compared to the ICC group, with anecdotal evidence. We found no difference between DCC and cut-UCM regarding the 3rd-minute PI, with moderate evidence.CONCLUSION: Umbilical clamping procedures (ICC, DCC, and cut-UCM) did not affect SpO2 and HR in the first ten minutes of life, but 3rd-minute PI values were slightly higher in DCC and cut-UCM compared with ICC among late preterm and term neonates.PMID:39002384 | DOI:10.1016/j.earlhumdev.2024.106075… -
Bacterial species in cord blood and their significance in the context of clinical use
Transfus Apher Sci. 2024 Aug;63(4):103961. doi: 10.1016/j.transci.2024.103961. Epub 2024 Jun 29.ABSTRACTApproximately 90 % of infants born before 28 full weeks(extremely-preterm-infants) receive erythrocyte transfusions in early life. Umbilical cord blood(UCB) has been investigated as an alternative source for erythrocyte transfusions to preterm neonates. This retrospective study aimed to compile/evaluate spectrum of bacteria groups/species intermittently detected in processed UCB at National-Swedish-Cord blood bank, (NS-CBB) during the years 2008-2020. Consecutive data from the years 2008-2020 were investigated. UCB from healthy newborns born after 37 full weeks of gestation was collected following clamping of cord (1 min) through cannulation of umbilical vein(vaginal-and C-section-deliveries). In total, 5194 cord blood units (UCBUs) that met NS-CBB-guidelines for total nucleated-cell-content(TNC) were manufactured from 8875 collections. Of 5194 UCBUs,77,6 % were from vaginal-and 22,4 % from C-section deliveries.Samples(10 mL) were collected from surplus eryhtrocyte fraction post-processing(n = 5194), transferred into BACT/ALERT® aerobic/anaerobic culture flasks and monitored 10 days using BACT/ALERT®-3D-Microbial-Detection-Systems. Positive samples were subcultured and typed for bacterial groups and/or species. Out of 5194 processed sampled UCB units,186 (3,6 %) were discarded due to positive sterility tests, 92 % were detected in samples from vaginal-deliveries and 8 % from C-section-deliveries. In all,16 different groups of bacteria and 27 species were identified. Common bacterial/groups and species were anaerobe gram-negative rods(n = 28),coagulase-negative-staphylococci(n = 21),gram-positive rods(n = 21),anaerobe-gram-positive cocci(n = 20) and viridans-streptococci(n = 13). Extracted from these results,in positive samples(n = 13) from C-section deliveries, bacteria were found:viridans-streptococci(n = 7),Aerococcus-urinae(n = 1), Staphylococcus lugdunensis(n = 1),other coagulase-negative staphylococci(n = 1) or a mix of aerobic/anaerobic bacteria(n = 3). Our results are in alignment with previously published contamination rates in processed UCBUs. Still, results point towards importance of strict microbial monitoring when manufacturing UCBUs to achieve patient-safe- products for stem-cell transplantation/transfusion.PMID:38981148 | DOI:10.1016/j.transci.2024.103961… -
Cord Obstruction and Delayed Cord Clamping Do Not Affect Gut Function in Neonatal Piglets
Neonatology. 2024 Jun 28:1-10. doi: 10.1159/000539527. Online ahead of print.ABSTRACTINTRODUCTION: Birth-related obstruction of umbilical blood flow may induce hypoxic insults that affect postnatal organ adaptation. Using newborn cesarean-delivered pigs, we hypothesized that cord obstruction during delivery negatively affects physiological transition and gut maturation. Further, we investigated if delayed cord clamping (DCC) improves gut outcomes, including sensitivity to formula-induced necrotizing enterocolitis (NEC)-like lesions.METHODS: In experiment 1, preterm (n = 24) and near-term (n = 29) piglets were subjected to umbilical cord obstruction (UCO, 5-7 min in utero), with corresponding pigs delivered without obstruction (CON, n = 17-22). Experiment 2 assessed preterm pigs subjected to delayed cord clamping (n = 30, 60 s) or immediate cord transection with umbilical cord milking (UCM, n = 34). Postnatal vital parameters were recorded, together with a series of gut parameters after 3 days of formula feeding.RESULTS: UCO induced respiratory-metabolic acidosis in near-term pigs at birth (pH 7.16 vs. 7.32, pCO2 12.5 vs. 9.2 kPa, lactate 5.2 vs. 2.5 mmol/L, p < 0.05). In preterm pigs, UCO increased failure of resuscitation and mortality shortly after birth (88 vs. 47%, p < 0.05). UCO did not affect gut permeability, transit time, macromolecule absorption, six digestive enzymes, or sensitivity to NEC-like lesions. In experiment 2, DCC improved neonatal hemodynamics (pH 7.28 vs. 7.20, pCO2 8.9 vs. 9.9 at 2 h, p < 0.05), with no effects on gut parameters.CONCLUSION: UCO and DCC affect neonatal transition and hemodynamics, but not neonatal gut adaptation or sensitivity to NEC-like lesions. Our findings suggest that the immature newborn gut is highly resilient to transient birth-related changes in cord blood flow.PMID:38952138 | DOI:10.1159/000539527… -
Two-Year Outcomes of Umbilical Cord Milking in Nonvigorous Infants: A Secondary Analysis of the MINVI Randomized Clinical Trial
JAMA Netw Open. 2024 Jul 1;7(7):e2416870. doi: 10.1001/jamanetworkopen.2024.16870.ABSTRACTIMPORTANCE: Compared with early cord clamping (ECC), umbilical cord milking (UCM) reduces delivery room cardiorespiratory support, hypoxic-ischemic encephalopathy, and therapeutic hypothermia in nonvigorous near-term and full-term infants. However, UCM postdischarge outcomes are not known.OBJECTIVE: To determine the 2-year outcomes of children randomized to UCM or ECC at birth in the Milking in Nonvigorous Infants (MINVI) trial.DESIGN, SETTING, AND PARTICIPANTS: A secondary analysis to evaluate longer-term outcomes of a cluster-randomized crossover trial was conducted from January 9, 2021, to September 25, 2023. The primary trial took place in 10 medical centers in the US, Canada, and Poland from January 5, 2019, to June 1, 2021, and hypothesized that UCM would reduce admission to the neonatal intensive care unit compared with ECC; follow-up concluded September 26, 2023. The population included near-term and full-term infants aged 35 to 42 weeks' gestation at birth who were nonvigorous; families provided consent to complete developmental screening questionnaires through age 2 years.INTERVENTION: UCM and ECC.MAIN OUTCOMES AND MEASURES: Ages and Stages Questionnaire, 3rd Edition (ASQ-3) and Modified Checklist for Autism in Toddlers, Revised/Follow-Up (M-CHAT-R/F) questionnaires at ages 22 to 26 months. Intention-to-treat analysis and per-protocol analyses were used.RESULTS: Among 1730 newborns from the primary trial, long-term outcomes were evaluated in 971 children (81%) who had ASQ-3 scores available at 2 years or died before age 2 years and 927 children (77%) who had M-CHAT-R/F scores or died before age 2 years. Maternal and neonatal characteristics by treatment group were similar, with median birth gestational age of 39 (IQR, 38-40) weeks in both groups; 224 infants (45%) in the UCM group and 201 (43%) in the ECC group were female. The median ASQ-3 total scores were similar (UCM: 255 [IQR, 225-280] vs ECC: 255 [IQR, 230-280]; P = .87), with no significant differences in the ASQ-3 subdomains. Medium- to high-risk M-CHAT-R/F scores were also similar (UCM, 9% [45 of 486] vs ECC, 8% [37 of 441]; P = .86).CONCLUSIONS AND RELEVANCE: In this secondary analysis of a randomized clinical trial among late near-term and full-term infants who were nonvigorous at birth, ASQ-3 scores at age 2 years were not significantly different between the UCM and ECC groups. Combined with previously reported important short-term benefits, this follow-up study suggests UCM is a feasible, no-cost intervention without longer-term neurodevelopmental risks of cord milking in nonvigorous near-term and term newborns.TRIAL REGISTRATION: ClinicalTrials.gov Identifier: NCT03631940.PMID:38949814 | PMC:PMC11217871 | DOI:10.1001/jamanetworkopen.2024.16870… -
Pregnancy Outcomes of Nifedipine Compared With Labetalol for Oral Treatment of Mild Chronic Hypertension
Obstet Gynecol. 2024 Jul 1;144(1):126-134. doi: 10.1097/AOG.0000000000005613. Epub 2024 May 23.ABSTRACTOBJECTIVE: To evaluate maternal and neonatal outcomes by type of antihypertensive used in participants of the CHAP (Chronic Hypertension in Pregnancy) trial.METHODS: We conducted a planned secondary analysis of CHAP, an open-label, multicenter, randomized trial of antihypertensive treatment compared with standard care (no treatment unless severe hypertension developed) in pregnant patients with mild chronic hypertension (blood pressure 140-159/90-104 mm Hg before 20 weeks of gestation) and singleton pregnancies. We performed three comparisons based on medications prescribed at enrollment: labetalol compared with standard care, nifedipine compared with standard care, and labetalol compared with nifedipine. Although active compared with standard care groups were randomized, medication assignment within the active treatment group was not random but based on clinician or patient preference. The primary outcome was the occurrence of superimposed preeclampsia with severe features, preterm birth before 35 weeks of gestation, placental abruption, or fetal or neonatal death. The key secondary outcome was small for gestational age (SGA) neonates. We also compared medication adverse effects between groups. Relative risks (RRs) and 95% CIs were estimated with log binomial regression to adjust for confounding.RESULTS: Of 2,292 participants analyzed, 720 (31.4%) received labetalol, 417 (18.2%) received nifedipine, and 1,155 (50.4%) received no treatment. The mean gestational age at enrollment was 10.5±3.7 weeks; nearly half of participants (47.5%) identified as non-Hispanic Black; and 44.5% used aspirin. The primary outcome occurred in 217 (30.1%), 130 (31.2%), and 427 (37.0%) in the labetalol, nifedipine, and standard care groups, respectively. Risk of the primary outcome was lower among those receiving treatment (labetalol use vs standard adjusted RR 0.82, 95% CI, 0.72-0.94; nifedipine use vs standard adjusted RR 0.84, 95% CI, 0.71-0.99), but there was no significant difference in risk when labetalol was compared with nifedipine (adjusted RR 0.98, 95% CI, 0.82-1.18). There were no significant differences in SGA or serious adverse events between participants receiving labetalol and those receiving nifedipine.CONCLUSION: No significant differences in predetermined maternal or neonatal outcomes were detected on the basis of the use of labetalol or nifedipine for treatment of chronic hypertension in pregnancy.CLINICAL TRIAL REGISTRATION: ClinicalTrials.gov, NCT02299414.PMID:38949541 | PMC:PMC11219006 | DOI:10.1097/AOG.0000000000005613… -
Management of Spontaneous Vaginal Delivery
Am Fam Physician. 2024 Jun;109(6):525-532.ABSTRACTPregnancy dating is determined by the patient's last menstrual period or an ultrasound measurement. A full-term pregnancy is considered 37 weeks' gestation or more. Spontaneous labor begins when regular painful uterine contractions result in a cervical change. Active labor begins at 6 cm dilation and is marked by more predictable, accelerated cervical change. In the absence of pregnancy complications, intermittent fetal auscultation may be considered as an alternative to continuous electronic fetal monitoring, which is associated with a high false-positive rate. Intravenous antibiotic prophylaxis is indicated in patients with group B streptococcus colonization or those at high risk to prevent newborn early-onset group B streptococcus. The likelihood of vaginal delivery is increased by providing continuous nonmedical support during labor, encouraging mobility, and using a peanut ball with epidural analgesia. Neuraxial analgesia is more effective for pain control than systemic opioids and is associated with fewer adverse effects. Delayed pushing during the second stage of labor has risks but does not affect the mode of delivery. Routine oropharyngeal suctioning of the newborn is not recommended, even with meconium-stained amniotic fluid. Delayed cord clamping reduces newborn anemia. Prevention of postpartum hemorrhage in patients at risk includes prophylactic uterotonic administration and controlled cord traction. Perineal lacerations that alter anatomy or are not hemostatic should be repaired. (Am Fam Physician. 2024;109(6):525-532.PMID:38905550… -
Impact of early versus delayed umbilical cord clamping on term neonates' haemoglobin levels: a randomized controlled trial
J Int Med Res. 2024 Jun;52(6):3000605241255836. doi: 10.1177/03000605241255836.ABSTRACTOBJECTIVE: To compare the effects of early and delayed cord clamping on the haemoglobin levels of neonates delivered at term.METHODS: This randomized controlled trial enrolled pregnant women during the second stage of labour. They were randomized into either the early cord clamping (ECC) group or the delayed cord clamping (DCC) group in the ratio of 1:1. Following delivery of the baby, the umbilical cords of participants in the ECC group were clamped within 30 s of delivery of the neonate while those of participants in the DCC group were clamped after 2 min from the delivery of the neonate. The primary outcome measure was the effect of ECC and DCC on the haemoglobin levels of neonates delivered at term.RESULTS: A total of 270 pregnant women were enrolled in the study. Their baseline sociodemographic and clinical characteristics were similar in both groups. There was no significant difference in the mean haemoglobin level between ECC and DCC groups at birth. The mean haemoglobin level of the neonates at 48 h postpartum was significantly higher in the DCC group than the ECC group.CONCLUSION: DCC at birth was associated with a significant increase in neonatal haemoglobin levels at 48 h postpartum when compared with ECC.Trial Registration: The trial was registered at Pan African Clinical Trial Registry with approval number PACTR202206735622089.PMID:38851870 | PMC:PMC11162598 | DOI:10.1177/03000605241255836… -
Comparison of Three Methods of Umbilical Cord Management in Late Preterm and Term Newborns on Hemoglobin and Ferritin Levels at Six Weeks of Age: A Randomized Controlled Trial
Cureus. 2024 Apr 26;16(4):e59046. doi: 10.7759/cureus.59046. eCollection 2024 Apr.ABSTRACTBACKGROUND: Umbilical cord milking (UCM) and delayed cord clamping (DCC) are strategies that improve the hemodynamic condition of the newborn and also increase the storage of iron. This study aimed to compare the effects of DCC with or without milking in late preterm and term neonates at different time intervals after birth (60, 120, and 180 seconds) on hematological and hemodynamic parameters in neonates at six weeks of age.MATERIALS AND METHODS: In this double-arm, parallel-group, triple-blind, and active-controlled trial, all 150 eligible neonates were randomized with allocation concealment into three groups: Group A (DCC with UCM at 60 seconds), Group B (DCC with UCM at 120 seconds), and Group C (only DCC for 180 seconds). Hemodynamic parameters were recorded and compared during the first 48 hours, and hematological parameters were compared at six weeks of age.RESULTS: At six weeks, a significant difference in hemoglobin levels was noted between Groups A, B, and C (p<0.001). The difference in serum ferritin values at six weeks was also statistically significant in comparisons across all three groups (p=0.003). Regarding secondary outcomes examined, hemodynamic parameters and the incidence of neonatal hyperbilirubinemia were found to be comparable at 48 hours after birth.CONCLUSION: DCC followed by UCM at 120 seconds and DCC till 180 seconds proves superior to DCC with UCM at 60 seconds in preserving elevated hemoglobin levels and iron stores in neonates at six weeks of age. DCC for 180 seconds yielded comparable results, followed by UCM at 120 seconds. All three methods are considered safe and effective without compromising the neonate's hemodynamics.PMID:38800297 | PMC:PMC11128072 | DOI:10.7759/cureus.59046… -
Mean Arterial Pressure and Neonatal Outcomes in Pregnancies Complicated by Mild Chronic Hypertension
Obstet Gynecol. 2024 Jul 1;144(1):101-108. doi: 10.1097/AOG.0000000000005611. Epub 2024 May 23.ABSTRACTOBJECTIVE: To estimate the association between mean arterial pressure during pregnancy and neonatal outcomes in participants with chronic hypertension using data from the CHAP (Chronic Hypertension and Pregnancy) trial.METHODS: A secondary analysis of the CHAP trial, an open-label, multicenter randomized trial of antihypertensive treatment in pregnancy, was conducted. The CHAP trial enrolled participants with mild chronic hypertension (blood pressure [BP] 140-159/90-104 mm Hg) and singleton pregnancies less than 23 weeks of gestation, randomizing them to active treatment (maintained on antihypertensive therapy with a goal BP below 140/90 mm Hg) or standard treatment (control; antihypertensives withheld unless BP reached 160 mm Hg systolic BP or higher or 105 mm Hg diastolic BP or higher). We used logistic regression to measure the strength of association between mean arterial pressure (average and highest across study visits) and to select neonatal outcomes. Unadjusted and adjusted odds ratios (per 1-unit increase in millimeters of mercury) of the primary neonatal composite outcome (bronchopulmonary dysplasia, retinopathy of prematurity, necrotizing enterocolitis, or intraventricular hemorrhage grade 3 or 4) and individual secondary outcomes (neonatal intensive care unit admission [NICU], low birth weight [LBW] below 2,500 g, and small for gestational age [SGA]) were calculated.RESULTS: A total of 2,284 participants were included: 1,155 active and 1,129 control. Adjusted models controlling for randomization group demonstrated that increasing average mean arterial pressure per millimeter of mercury was associated with an increase in each neonatal outcome examined except NEC, specifically neonatal composite (adjusted odds ratio [aOR] 1.12, 95% CI, 1.09-1.16), NICU admission (aOR 1.07, 95% CI, 1.06-1.08), LBW (aOR 1.12, 95% CI, 1.11-1.14), SGA below the fifth percentile (aOR 1.03, 95% CI, 1.01-1.06), and SGA below the 10th percentile (aOR 1.02, 95% CI, 1.01-1.04). Models using the highest mean arterial pressure as opposed to average mean arterial pressure also demonstrated consistent associations.CONCLUSION: Increasing mean arterial pressure was positively associated with most adverse neonatal outcomes except NEC. Given that the relationship between mean arterial pressure and adverse pregnancy outcomes may not be consistent at all mean arterial pressure levels, future work should attempt to further elucidate whether there is an absolute threshold or relative change in mean arterial pressure at which fetal benefits are optimized along with maternal benefits.CLINICAL TRIAL REGISTRATION: ClinicalTrials.gov , NCT02299414.PMID:38781591 | PMC:PMC11216857 | DOI:10.1097/AOG.0000000000005611… -
Measuring direct effect of cord clamping approaches: getting the right target group
Pediatr Res. 2024 Jul;96(1):5-6. doi: 10.1038/s41390-024-03284-3. Epub 2024 May 20.NO ABSTRACTPMID:38769402 | DOI:10.1038/s41390-024-03284-3… -
Ventilatory Assistance Before Umbilical Cord Clamping in Extremely Preterm Infants: A Randomized Clinical Trial
JAMA Netw Open. 2024 May 1;7(5):e2411140. doi: 10.1001/jamanetworkopen.2024.11140.ABSTRACTIMPORTANCE: Providing assisted ventilation during delayed umbilical cord clamping may improve outcomes for extremely preterm infants.OBJECTIVE: To determine whether assisted ventilation in extremely preterm infants (23 0/7 to 28 6/7 weeks' gestational age [GA]) followed by cord clamping reduces intraventricular hemorrhage (IVH) or early death.DESIGN, SETTING, AND PARTICIPANTS: This phase 3, 1:1, parallel-stratified randomized clinical trial conducted at 12 perinatal centers across the US and Canada from September 2, 2016, through February 21, 2023, assessed IVH and early death outcomes of extremely preterm infants randomized to receive 120 seconds of assisted ventilation followed by cord clamping vs delayed cord clamping for 30 to 60 seconds with ventilatory assistance afterward. Two analysis cohorts, not breathing well and breathing well, were specified a priori based on assessment of breathing 30 seconds after birth.INTERVENTION: After birth, all infants received stimulation and suctioning if needed. From 30 to 120 seconds, infants randomized to the intervention received continuous positive airway pressure if breathing well or positive-pressure ventilation if not, with cord clamping at 120 seconds. Control infants received 30 to 60 seconds of delayed cord clamping followed by standard resuscitation.MAIN OUTCOMES AND MEASURES: The primary outcome was any grade IVH on head ultrasonography or death before day 7. Interpretation by site radiologists was confirmed by independent radiologists, all masked to study group. To estimate the association between study group and outcome, data were analyzed using the stratified Cochran-Mantel-Haenszel test for relative risk (RR), with associations summarized by point estimates and 95% CIs.RESULTS: Of 1110 women who consented to participate, 548 were randomized and delivered infants at GA less than 29 weeks. A total of 570 eligible infants were enrolled (median [IQR] GA, 26.6 [24.9-27.7] weeks; 297 male [52.1%]). Intraventricular hemorrhage or death occurred in 34.9% (97 of 278) of infants in the intervention group and 32.5% (95 of 292) in the control group (adjusted RR, 1.02; 95% CI, 0.81-1.27). In the prespecified not-breathing-well cohort (47.5% [271 of 570]; median [IQR] GA, 26.0 [24.7-27.4] weeks; 152 male [56.1%]), IVH or death occurred in 38.7% (58 of 150) of infants in the intervention group and 43.0% (52 of 121) in the control group (RR, 0.91; 95% CI, 0.68-1.21). There was no evidence of differences in death, severe brain injury, or major morbidities between the intervention and control groups in either breathing cohort.CONCLUSIONS AND RELEVANCE: This study did not show that providing assisted ventilation before cord clamping in extremely preterm infants reduces IVH or early death. Additional study around the feasibility, safety, and efficacy of assisted ventilation before cord clamping may provide additional insight.TRIAL REGISTRATION: ClinicalTrials.gov Identifier: NCT02742454.PMID:38758557 | PMC:PMC11102017 | DOI:10.1001/jamanetworkopen.2024.11140… -
Effect of administration routes of oxytocin on hemoglobin in neonates with delayed umbilical cord clamping: a multi-centre randomized controlled clinical trial
Arch Gynecol Obstet. 2024 Aug;310(2):991-999. doi: 10.1007/s00404-024-07543-w. Epub 2024 May 16.ABSTRACTPURPOSE: To evaluate the effect of intravenous infusion versus intramyometrial injection of oxytocin on hemoglobin levels in neonates with delayed umbilical cord clamping during cesarean section.METHODS: The multi-centre randomized controlled trial was performed at three hospitals from February to June 2023. Women with term singleton gestations scheduled for cesarean delivery were allocated to receive an intravenous infusion of 10 units of oxytocin or a myometrial injection of 10 units of oxytocin during the surgery. The primary outcome was neonatal hemoglobin at 48 to 96 h after birth. Secondary outcomes were side-effects of oxytocin, postpartum haemorrhage, phototherapy for jaundice, feeding at 1 month, maternal and neonatal morbidity and re-admissions.RESULTS: A total of 360 women were randomized (180 women in each group). The mean neonatal hemoglobin did not show a significant difference between the intravenous infusion group (194.3 ± 21.7 g/L) and the intramyometrial groups (195.2 ± 24.3 g/L) (p = 0.715). Secondary neonatal outcomes, involving phototherapy for jaundice, feeding at 1 month and neonatal intensive care unit admission were similar between the two groups. The maternal outcomes did not differ significantly between the two groups, except for a 200 mL higher intraoperative infusion volume observed in the intravenous group compared to the intramyometrial group.CONCLUSION: Among women undergoing elective cesarean delivery of term singleton pregnancies, there was no significant difference in neonatal hemoglobin at 48 to 96 h after birth between infants with delayed cord clamping, whether the oxytocin was administrated by intravenous infusion or intramyometrial injection.TRIAL REGISTRATION: Chinese Clinical trial registry: ChiCTR2300067953 (1 February 2023).PMID:38753205 | PMC:PMC11258157 | DOI:10.1007/s00404-024-07543-w… -
Neonatal Resuscitation Practices in Portuguese Delivery Rooms: A Cross-Sectional Study
Acta Med Port. 2024 May 2;37(5):342-354. doi: 10.20344/amp.20009. Epub 2024 May 2.ABSTRACTINTRODUCTION: Data from previous studies have demonstrated inconsistency between current evidence and delivery room resuscitation practices in developed countries. The primary aim of this study was to assess the quality of newborn healthcare and resuscitation practices in Portuguese delivery rooms, comparing current practices with the 2021 European Resuscitation Council guidelines. The secondary aim was to compare the consistency of practices between tertiary and non-tertiary centers across Portugal.METHODS: An 87-question survey concerning neonatal care was sent to all physicians registered with the Portuguese Neonatal Society via email. In order to compare practices between centers, participants were divided into two groups: Group A (level III and level IIb centers) and Group B (level IIa and I centers). A descriptive analysis of variables was performed in order to compare the two groups.RESULTS: In total, 130 physicians responded to the survey. Group A included 91 (70%) and Group B 39 (30%) respondents. More than 80% of participants reported the presence of a healthcare professional with basic newborn resuscitation training in all deliveries, essential equipment in the delivery room, such as a resuscitator with a light and heat source, a pulse oximeter, and an O2 blender, and performing delayed cord clamping for all neonates born without complications. Less than 60% reported performing team briefing before deliveries, the presence of electrocardiogram sensors, end-tidal CO2 detector, and continuous positive airway pressure in the delivery room, and monitoring the neonate's temperature. Major differences between groups were found regarding staff attending deliveries, education, equipment, thermal control, umbilical cord management, vital signs monitoring, prophylactic surfactant administration, and the neonate's transportation out of the delivery room.CONCLUSION: Overall, adherence to neonatal resuscitation international guidelines was high among Portuguese physicians. However, differences between guidelines and current practices, as well as between centers with different levels of care, were identified. Areas for improvement include team briefing, ethics, education, available equipment in delivery rooms, temperature control, and airway management. The authors emphasize the importance of continuous education to ensure compliance with the most recent guidelines and ultimately improve neonatal health outcomes.PMID:38744237 | DOI:10.20344/amp.20009… -
Newborns at risk of COVID-19, the story continues
J Perinat Med. 2024 May 15;52(6):567-574. doi: 10.1515/jpm-2024-0125. Print 2024 Jul 26.ABSTRACTAfter more than 4 years of the SARS-CoV-2 pandemic, a great deal of knowledge on how this virus affects pregnant women, the fetus and the newborn has accumulated. Guidelines for mode of delivery, cord clamping, skin to skin, breastfeeding, and rooming-in have become uniform across the world. Vaccination has considerably improved outcomes, but hesitancy amongst pregnant patients and the emergence of variants remain challenged and SARS-CoV-2 positivity during pregnancy continues to be associated with an increased risk of maternal complications, premature delivery and higher neonatal mortality and morbidity. An emerging body of data now exists on the effect of SARS-CoV-2 in pregnancy on early neonatal outcomes, medical education in obstetrics and pediatrics, and longer-term developmental outcomes. In this article, we review the development in this field since our last review.PMID:38742624 | DOI:10.1515/jpm-2024-0125… -
Effect of Delayed Cord Clamping on Breastfeeding Behaviors During the First Breastfeed: A Randomized Controlled Study
Breastfeed Med. 2024 Aug;19(8):624-628. doi: 10.1089/bfm.2024.0080. Epub 2024 May 13.ABSTRACTObjective: Delayed cord clamping (DCC) may increase the success of breastfeeding by improving neurological and cardiovascular function in neonates. In this study, we investigated the impact of DCC on breastfeeding behaviors, neonatal activity status, and maternal satisfaction during the first breastfeeding. Methods: This randomized controlled study was conducted in a tertiary hospital in Turkey with 100 term infants delivered by elective cesarean section with spinal anesthesia. The participants were randomly assigned to the early cord clamping (ECC) group or DCC group. The Infant Breastfeeding Assessment Tool (IBFAT) was used to assess infant alertness, breastfeeding behaviors, and maternal satisfaction with breastfeeding within the first 2 hours of life. Results: Scores on the IBFAT were significantly higher in the DCC group compared with the ECC group (p = 0.02). Maternal satisfaction with breastfeeding did not differ between the groups (p = 0.3). Infant alertness tended to be better in the DCC group, but the difference was not statistically significant (p = 0.08). Conclusion: The results of this study indicated that DCC was associated with more favorable breastfeeding behaviors compared with ECC.PMID:38738940 | DOI:10.1089/bfm.2024.0080… -
Persistent omphalomesenteric duct in an infant with trisomy 21
BMJ Case Rep. 2024 May 8;17(5):e259671. doi: 10.1136/bcr-2024-259671.ABSTRACTWe present the case of a term newborn with trisomy 21 who presented to the paediatric emergency department with periumbilical flare and green-brown discharge from a clamped umbilical cord, initially suspected to be omphalitis. However, it was noticed later, that when the infant strained or cried, a thick, bubbling and offensive green-brown discharge came out of the clamped umbilical cord with umbilical flatus. An ultrasound abdomen and umbilical cord confirmed the presence of a persistent omphalomesenteric duct (POMD). He was then transferred to the paediatric surgical unit. There, he underwent a laparotomy and surgical resection of the POMD and was discharged home 2 days later.PMID:38719262 | PMC:PMC11085785 | DOI:10.1136/bcr-2024-259671… -
OBSTRUCTED CONGENITAL HERNIA OF UMBILICAL CORD IN A NIGERIAN NEWBORN AND ITS DIAGNOSTIC CONUNDRUM
Ann Ib Postgrad Med. 2023 Dec;21(3):75-78. Epub 2024 Jan 30.ABSTRACTBACKGROUND: Congenital Hernia of umbilical cord (CHUC) is a rare presentation. The failure of return of intestinal loops following physiological herniation has been postulated as the embryological basis of this condition. This is usually mistakenly termed as omphalocele minor. We aim to highlight this rare finding, the clinical features, diagnostic dilemma, and management of CHUC.CASE PRESENTATION: He is a 4-day old male with obstructed CHUC. He had an oedematous umbilical stump, with circumferential normal abdominal wall skin folds in the form of a collar wrapping round the proximal aspect of the protrusion. The umbilical defect measured about 4 cm in diameter. Subsequently, surgical reduction and repair of defect was done, with resolution of symptoms.CONCLUSION: CHUC though a rare entity and easily missed, accurate diagnosis and management offer good prognosis. Also, recognition will prevent iatrogenic bowel injury from careless clamping of the cord with associated morbidity and mortality. It also helps to prevent mis categorization and prevent unwarranted anxiety with misdiagnosis.PMID:38706623 | PMC:PMC11065190… -
Quality improvement efforts directed at optimal umbilical cord management in delivery room
Semin Perinatol. 2024 Apr;48(3):151905. doi: 10.1016/j.semperi.2024.151905. Epub 2024 Apr 19.ABSTRACTDelayed or deferred cord clamping (DCC) and umbilical cord milking (UCM) benefit all infants by optimizing fetal-neonatal transition and placental transfusion. Even though DCC is recommended by almost all maternal and neonatal organizations, it has not been universally implemented. There is considerable variation in umbilical cord management practices across institutions. In this article, we provide examples of successful quality improvement (QI) initiatives to implement optimal cord management in the delivery room. We discuss a number of key elements that should be considering among those undertaking QI efforts to implement DCC and UCM including, multidisciplinary team collaboration, development of theory for change, mapping of the current and ideal process and workflow for cord management, and creation of a unit-specific evidence-based protocol for cord management. We also examine important strategies for implementation and provide suggestions for developing a system for measurement and benchmarking.PMID:38679508 | DOI:10.1016/j.semperi.2024.151905… -
How does maternal anemia affect the levels of umbilical cord brain-derived neurotrophic factor?
Eur J Obstet Gynecol Reprod Biol. 2024 Jun;297:182-186. doi: 10.1016/j.ejogrb.2024.04.016. Epub 2024 Apr 19.ABSTRACTOBJECTIVE: In this study, we aimed to evaluate the effect of maternal iron deficiency anemia on the umbilical cord level of brain-derived neurotrophic factor (BDNF), which plays a very important role in the central nervous system.METHODS: Our research was planned as a quantitative, prospective, and analytical type of study. A total of 90 volunteers, term, singleton pregnant hospitalized in the Health Sciences University Ümraniye Training and Research Hospital Gynecology and Obstetrics Clinic between September 2021 and August 2022 were included in this study. While 45 of these pregnants were pregnant women with iron deficiency anemia (hemoglobin ≤ 110 g/L and serum ferritin level ≤ 12 μg/L), 45 cases were in the control group without iron deficiency anemia (hemoglobin > 110 g/L, serum ferritin > 12 μg/L). When pregnant were admitted to the hospital, blood samples were taken to analyze hemoglobin, mean cell volume (MCV), iron, unsaturated iron binding capacity, total iron binding capacity, serum ferritin, transferrin, and CRP levels. Also, we noted the maternal age, gravida, parity, birth weight, head circumference, type of birth, 1. minute Apgar score, and 5. minute Apgar score. During the delivery; after the umbilical cord had been clamped and cut, we took 5 cc of umbilical cord blood. Then, we put it in the serum-separating laboratory tubes. After we centrifuged these blood samples, we put the serum parts in the Eppendorf tubes to be stored at -80 degrees Celsius. At the end of the study, we calculated the level of BDNF using special human brain-derived neurotrophic factor ELISA kits. The umbilical cord BDNF levels of the maternal iron deficiency anemia group and the control group were compared statistically.RESULTS: When we evaluated the fetal umbilical cord BDNF values of 90 participants, the median value BDNF in the babies of 45 anemic mothers was 3.16 (IQR 0.73), and the median BDNF value of the babies of 45 healthy mothers was 5.37 (IQR 1.02). We found a statistical difference between BDNF and hemoglobin, hematocrit, MCV, and iron values between these two groups.CONCLUSION: In conclusion, the BDNF value of the babies of healthy individuals is higher than that of anemic individuals. Our study showed that the amount of BDNF in the umbilical cord blood was significantly affected by maternal iron deficiency anemia.PMID:38677095 | DOI:10.1016/j.ejogrb.2024.04.016… -
Does delayed cord clamping result in higher maternal blood loss in primary cesarean sections? A retrospective comparative study
J Perinat Med. 2024 Apr 29;52(5):494-500. doi: 10.1515/jpm-2023-0450. Print 2024 Jun 25.ABSTRACTOBJECTIVES: The University Hospital Basel implemented delayed umbilical cord clamping of 30-60 s in all laboring women on April 1, 2020. This practice has been widely researched showing substantial benefit for the neonate. Few studies focused on maternal blood loss. The objective of our retrospective comparative study was to assess the impact of immediate vs. delayed cord clamping on maternal blood loss in primary scheduled cesarean sections.METHODS: We analyzed data of 98 women with singleton gestations undergoing primary scheduled cesarean section at term. Data from procedures with early cord clamping (ECC) were compared to those after implementation of delayed cord clamping (DCC). Primary outcomes were perioperative change in maternal hemoglobin levels, estimated and calculated blood loss. Secondary outcomes included duration of cesarean section and neonatal data.RESULTS: There was a statistically significant difference in the mean perioperative decline of hemoglobin of 10.4 g/L (SD=7.92) and 18.7 g/L (SD=10.4) between the ECC and DCC group, respectively (p<0.001). The estimated (482 mL in ECC vs. 566 mL in DCC (p=0.011)) and the calculated blood loss (438 mL in ECC vs. 715 mL in DCC (p=0.002)) also differed significantly. Secondary outcomes showed no significant differences.CONCLUSIONS: In our study DCC resulted in a statistically significant higher maternal blood loss. In our opinion the widely researched neonatal benefit of DCC outweighs the risk of higher maternal blood loss in low-risk patients. However, maternal risks must be minimized, improvements to preoperative blood management and operative techniques are required.PMID:38676940 | DOI:10.1515/jpm-2023-0450… -
Blood pressure and cerebral oxygenation with physiologically-based cord clamping: sub-study of the BabyDUCC trial
Pediatr Res. 2024 Jul;96(1):124-131. doi: 10.1038/s41390-024-03131-5. Epub 2024 Apr 26.ABSTRACTBACKGROUND: Cord-clamping strategies may modify blood pressure (BP) and cerebral tissue oxygen saturation (rStO2) immediately after birth.METHODS: We conducted a sub-study nested within the Baby-Directed Umbilical Cord-Clamping trial. Infants ≥32+0 weeks' gestation assessed as requiring resuscitation were randomly allocated to either physiologically-based cord clamping (PBCC), where resuscitation commenced prior to umbilical cord clamping, or standard care where cord clamping occurred early (ECC). In this single-site sub-study, we obtained additional measurements of pre-ductal BP and rStO2. In a separate observational arm, non-randomised vigorous infants received 2 min of deferred cord clamping (DCC) and contributed data for reference percentiles.RESULTS: Among 161 included infants, n = 55 were randomly allocated to PBCC (n = 30) or ECC (n = 25). The mean (SD) BP at 3-4 min after birth (primary outcome) in the PBCC group was 64 (10) mmHg compared to 62 (10) mmHg in the ECC group, mean difference 2 mmHg (95% confidence interval -3-8 mmHg, p = 0.42). BP and rStO2 were similar across both randomised arms and the observational arm (n = 106).CONCLUSION: We found no difference in BP or rStO2 with the different cord clamping strategies. We report reference ranges for BP and rStO2 for late-preterm and full-term infants receiving DCC.IMPACT: Among late-preterm and full-term infants receiving varying levels of resuscitation, blood pressure (BP, at 3-4 minutes and 6 min) and cerebral tissue oxygen saturation (rStO2) are not influenced by timing of cord clamping in relation to establishment of ventilation. Infants in this study did not require advanced resuscitation, where cord clamping strategies may yet influence BP and rStO2. The reference ranges for BP and rStO2 represent the first, to our knowledge, for vigorous late-preterm and full-term infants receiving deferred cord clamping. rStO2 > 90% (~90th percentile) may be used to define cerebral hyperoxia, for instance when studying oxygen supplementation after birth.PMID:38671085 | PMC:PMC11257956 | DOI:10.1038/s41390-024-03131-5… -
Impact of shared decision-making on women's childbirth preferences: A cluster randomised controlled trial
Midwifery. 2024 Jun;133:103999. doi: 10.1016/j.midw.2024.103999. Epub 2024 Apr 12.ABSTRACTBACKGROUND: Midwives provide counselling for birth plans (BPs) to women during prenatal care; however, the impact of individualised BP counselling interventions based on shared decision-making (SDM) regarding women's preferences is unknown.METHODS: This randomised cluster trial included four primary healthcare units. Midwives provided BP counselling based on SDM to women in the intervention group (IG) during prenatal care along with a handout about evidence-based recommendations. Women in the control group (CG) received standard BP counselling from midwives. The main outcome was preference changes concerning BPs.RESULTS: A total of 461 (95.5 %) pregnant women received BP counselling (IG, n = 247; CG, n = 214). Women in the IG changed their BP preferences for 13 items compared with those in the CG. These items were: using an unique space during birth (81.1 % vs 51.6 %; p < 0.001), option for light graduation (63 % vs 44.7 %; p < 0.001), listening to music (57.3 % vs 43.6 %; p = 0.006), drinking fluids during labour (84.6 % vs 93.6 %; p = 0.005), continuous monitoring (59 % vs 37.8 %; p < 0.001); desire for natural childbirth (36.6 % vs 25 %; p = 0.014), epidural analgesia (55.1 % vs 43.6 %; p = 0.023); breathing techniques (65.2 % vs 50.5 %; p = 0.003), massage (74.9 % vs 55.3 %; p < 0.001); birthing ball use (81.9 % vs 56.9 %; p < 0.001), spontaneous pushing (49.3 % vs 28.7 %; p < 0.001), choosing birth position (69.6 % vs 41.5 %) and delayed umbilical cord clamping (67.8 % vs 44.1 %; p = 0.001).CONCLUSION: SDM counselling, together with a handout about evidence-based recommendations on childbirth and newborn care, produced more changes in women's preferences expressed in the BP than standard counselling.PMID:38643600 | DOI:10.1016/j.midw.2024.103999… -
Delayed cord clamping and the response to bradycardia immediately after birth
Arch Dis Child Fetal Neonatal Ed. 2024 Jun 19;109(4):346-347. doi: 10.1136/archdischild-2023-326398.NO ABSTRACTPMID:38641420 | DOI:10.1136/archdischild-2023-326398… -
Deferred cord clamping and polythene bags at delivery: measuring and improving quality
Arch Dis Child Fetal Neonatal Ed. 2024 Jun 19;109(4):344-345. doi: 10.1136/archdischild-2023-326702.NO ABSTRACTPMID:38641419 | DOI:10.1136/archdischild-2023-326702… -
Achieving optimal cord management: a multidisciplinary quality improvement initiative
BMJ Open Qual. 2024 Apr 15;13(2):e002662. doi: 10.1136/bmjoq-2023-002662.ABSTRACTOptimal cord management (OCM), defined as waiting at least 60 seconds (s) before clamping the umbilical cord after birth, is an evidence-based intervention that improves outcomes for both term and preterm babies. All major resuscitation councils recommend OCM for well newborns.National Neonatal Audit Programme (NNAP) benchmarking data identified our tertiary neonatal unit as a negative outlier with regard to OCM practice with only 12.1% of infants receiving the recommended minimum of 60 s. This inspired a quality improvement project (QIP) to increase OCM rates of ≥ 60 s for infants <34 weeks. A multidisciplinary QIP team (Neonatal medical and nursing staff, Obstetricians, Midwives and Anaesthetic colleagues) was formed, and robust evidence-based quality improvement methodologies employed. Our aim was to increase OCM of ≥ 60 s for infants born at <34 weeks to at least 40%.The percentage of infants <34 weeks receiving OCM increased from 32.4% at baseline (June-September 2022) to 73.6% in the 9 months following QIP commencement (October 2022-June 2023). The intervention period spanned two cohorts of rotational doctors, demonstrating its sustainability. Rates of admission normothermia were maintained following the routine adoption of OCM (89.2% vs 88.5%), which is a complication described by other neonatal units.This project demonstrates the power of a multidisciplinary team approach to embedding an intervention that relies on collaboration between multiple departments. It also highlights the importance of national benchmarking data in allowing departments to focus QIP efforts to achieve long-lasting transformational service improvements.PMID:38626936 | PMC:PMC11029183 | DOI:10.1136/bmjoq-2023-002662… -
Successful management of fetal hypoxia due to amniotic banding at 26 weeks of pregnancy: A case report of a rare survival
Eur J Obstet Gynecol Reprod Biol. 2024 Jun;297:264-266. doi: 10.1016/j.ejogrb.2024.04.010. Epub 2024 Apr 14.ABSTRACTBACKGROUND: Amniotic banding is a rare condition that can lead to structural limb anomalies, fetal distress and adverse obstetric outcomes. The main hypothesis for its etiology is a rupture of the amniotic membrane in early pregnancy, with the formation of tightly entangling strands around the fetus. These strands can constrict, incise, and subsequently amputate limb parts, the neck or head. More rarely, the amniotic banding can affect the umbilical cord, leading to fetal distress or potential intra-uterine fetal demise.OBJECTIVE: We present a unique case of a 26-week pregnant woman who attended a polyclinical consultation due to reduced fetal movements with concerning cardiotocography (CTG) findings. A review of the literature about amniotic banding of the umbilical cord was conducted as well, identifying diagnostic and interventional options for the obstetrician's practice.STUDY DESIGN: This is a case report, alongside a review of the literature.RESULTS: The CTG indicated fetal distress, prompting an emergency caesarean section (C-section). Upon delivery, the neonate exhibited signs of amniotic band sequence, with distal phalangeal defects on the right hand and severe constriction of the umbilical cord caused by amniotic strands, the latter precipitating fetal hypoxia. Direct ultrasound diagnosis remains a challenge in the absence of limb amputation, yet indirect signs such as distal limb or umbilical doppler flow abnormalities and distal limb edema may be suggestive of amniotic banding. MRI is proposed as an adjuvant diagnostic tool yet does not present a higher detection rate compared to ultrasound. Fetoscopic surgery to perform lysis of the amniotic strands with favorable outcome has been described in literature.CONCLUSION: This case presents the first reported survival of an extremely preterm fetus in hypoxic distress as a cause of amniotic banding of the umbilical cord, with a rare degree of incidental timing. Ultrasound diagnosis remains the gold standard. Obstetrical vigilance is warranted, with fetal rescue proven to be feasible.PMID:38616145 | DOI:10.1016/j.ejogrb.2024.04.010… -
Influence of umbilical cord clamping time on cerebral oxygenation and early cardiac function in term infants
J Neonatal Perinatal Med. 2024;17(4):535-542. doi: 10.3233/NPM-230223.ABSTRACTBACKGROUND: Delayed cord clamping is the standard of care for both term and preterm infants worldwide. The aim of this study was to evaluate the effect of 60-second or 180-second delayed cord clamping during labor on cerebral oxygenation and cardiac function.METHODS: Healthy newborns were divided into two groups: a 60-second delay in cord clamping (60-s DCC) and a 180-second delay in cord clamping (180-s DCC) at birth. Pulse oximetry and cerebral near-infrared spectroscopy (cNIRS) probes were placed during postnatal care. A total of 84 healthy newborns were included in this study. Preductal oxygen saturation (SpO2), heart rate, and cNIRS values were recorded at 5 and 10 minutes after delivery. The cardiac function of the infants was assessed by echocardiography at 3-7 days postnatally.RESULTS: There was no significant difference between the groups in SpO2 and cNIRS values at 5 and 10 min. While there was no significant difference in the number of neonates with targeted SpO2 at the 5th and 10th min and targeted cNIRS values at the 10th min, there was a significant difference in the number of neonates with target cNIRS values at the 5th min between groups (p < 0.001). Echocardiographic findings showed that pulmonary flow velocity was increased in the 180-s DCC group; the difference was statistically significant (p = 0.04).CONCLUSION: Our results showed that the number of infants with normal cNIRS values regarding cerebral oxygenation was higher in the 180-s DCC group. The pulmonary flow velocity was significantly increased in the 180-s DCC group in terms of echocardiographic findings.PMID:38607769 | DOI:10.3233/NPM-230223… -
How long is too long? No added benefit with prolonged ventilation with intact cord in preterm infants
J Physiol. 2024 Apr;602(8):1663-1664. doi: 10.1113/JP286492. Epub 2024 Apr 11.NO ABSTRACTPMID:38602842 | PMC:PMC11090468 | DOI:10.1113/JP286492… -
Umbilical cord milking and delayed cord clamping for the prevention of neonatal hypoglycaemia: a systematic review and meta-analysis
BMC Pregnancy Childbirth. 2024 Apr 8;24(1):248. doi: 10.1186/s12884-024-06427-w.ABSTRACTBACKGROUND: Placental management strategies such as umbilical cord milking and delayed cord clamping may provide a range of benefits for the newborn. The aim of this review was to assess the effectiveness of umbilical cord milking and delayed cord clamping for the prevention of neonatal hypoglycaemia.METHODS: Three databases and five clinical trial registries were systematically reviewed to identify randomised controlled trials comparing umbilical cord milking or delayed cord clamping with control in term and preterm infants. The primary outcome was neonatal hypoglycaemia (study defined). Two independent reviewers conducted screening, data extraction and quality assessment. Quality of the included studies was assessed using the Cochrane Risk of Bias tool (RoB-2). Certainty of evidence was assessed using the Grading of Recommendations, Assessment, Development and Evaluation (GRADE) approach. Meta-analysis using a random effect model was done using Review Manager 5.4. The review was registered prospectively on PROSPERO (CRD42022356553).RESULTS: Data from 71 studies and 14 268 infants were included in this review; 22 (2 537 infants) compared umbilical cord milking with control, and 50 studies (11 731 infants) compared delayed with early cord clamping. For umbilical cord milking there were no data on neonatal hypoglycaemia, and no differences between groups for any of the secondary outcomes. We found no evidence that delayed cord clamping reduced the incidence of hypoglycaemia (6 studies, 444 infants, RR = 0.87, CI: 0.58 to 1.30, p = 0.49, I2 = 0%). Delayed cord clamping was associated with a 27% reduction in neonatal mortality (15 studies, 3 041 infants, RR = 0.73, CI: 0.55 to 0.98, p = 0.03, I2 = 0%). We found no evidence for the effect of delayed cord clamping for any of the other outcomes. The certainty of evidence was low for all outcomes.CONCLUSION: We found no data for the effectiveness of umbilical cord milking on neonatal hypoglycaemia, and no evidence that delayed cord clamping reduced the incidence of hypoglycaemia, but the certainty of the evidence was low.PMID:38589786 | PMC:PMC11000397 | DOI:10.1186/s12884-024-06427-w… -
A randomised controlled trial comparing umbilical cord milking to delayed cord clamping at birth in preterm infants 28-36 weeks gestational age
Eur J Pediatr. 2024 Jun;183(6):2791-2796. doi: 10.1007/s00431-024-05550-2. Epub 2024 Apr 6.ABSTRACTDelayed cord clamping (DCC) is an established practice in perinatology with multiple benefits. However, in instances where the implementation of DCC is not viable, it needs alternatives, especially during caesarean deliveries. A non-inferiority randomized, non-blinded, trial was conducted at a tertiary care referral unit in South India among the preterm newborns (28-36 weeks) randomized to DCC as opposed to intact-umbilical cord milking (UCM). The primary objective was to compare the mean haemoglobin values between the two groups, and the secondary outcome was to compare death and/or major IVH (> Grade II). Of the 132 eligible newborn infants, 99 were randomized to two study groups. Of the 59 and 40 randomised to UCM and DCC, 54 and 36 received the allocated intervention respectively. Preterm infants who underwent UCM had significantly higher haemoglobin (19.97 ± 1.44) as compared to DCC group (18.62 ± 0.98) p-0.0001. The rates of mortality and/or major IVH were comparable between the two groups.CONCLUSION: UCM may be a feasible alternative to DCC especially in settings where the latter is not achievable, without increasing the risk of adverse effects to the preterm infants, this finding needing further confirmation with larger sample.TRIAL REGISTRATION: CTRI (Clinical Trial Registry-India) registration number: CTRI/2020/04/024566 (registered prospectively on 13/04/2020).WHAT IS KNOWN: • Delayed cord clamping (DCC) is recommended as a standard of care for all the stable term and preterm newborn babies at birth.WHAT IS NEW: • Intact umbilical cord milking may be a reasonable choice of cord management when DCC is unsuccessful, without increasing adverse effects for the new born.PMID:38581461 | DOI:10.1007/s00431-024-05550-2… -
Relationship between the natural cessation time of umbilical cord pulsation in full-term newborns delivered vaginally and maternal-neonatal outcomes: a prospective cohort study
BMC Pregnancy Childbirth. 2024 Apr 4;24(1):236. doi: 10.1186/s12884-024-06444-9.ABSTRACTBACKGROUND: To analyze the impact of the time of natural cessation of the umbilical cord on maternal and infant outcomes in order to explore the time of clamping that would be beneficial to maternal and infant outcomes.METHODS: The study was a cohort study and pregnant women who met the inclusion and exclusion criteria at the Obstetrics and Gynecology Department of Qilu Hospital of Shandong University from September 2020 to September 2021. Analysis using Kruskal-Wallis rank sum test, Pearson's Chi-squared test, generalized linear mixed model (GLMM) and repeated measures ANOVA. If the difference between groups was statistically significant, the Bonferroni test was then performed. A two-sided test of P < 0.05 was considered statistically significant.RESULTS: A total of 345 pregnants were included in this study. The subjects were divided into the ≤60 seconds group (n = 134), the 61-89 seconds group (n = 106) and the ≥90 seconds group (n = 105) according to the time of natural arrest of the umbilical cord. There was no statistically significant difference in the amount of postpartum hemorrhage and the need for iron, medication, or supplements in the postpartum period between the different cord spontaneous arrest time groups for mothers (P > 0.05). The weight of the newborns in the three groups was (3316.27 ± 356.70) g, (3387.26 ± 379.20) g, and (3455.52 ± 363.78) g, respectively, and the number of days of cord detachment was 12.00 (8.00, 15.75) days, 10.00 (7.00, 15.00) days and 9.00 (7.00, 13.00) days, respectively, as the time of natural cessation of the cord increased. The neonatal lymphocyte ratio, erythrocyte pressure, and hemoglobin reached a maximum in the 61-89 s group at (7.41 ± 2.16) %, (61.77 ± 8.17) % and (194.52 ± 25.84) g/L, respectively. Lower incidence of neonatal hyperbilirubinemia in the 61-89 s group compared to the ≥90s group 0 vs 4.8 (P < 0.05).CONCLUSIONS: In full-term singleton vaginal births, maternal and infant outcomes are better when waiting for 61-89 s after birth for the cord to stop pulsating naturally, suggesting that we can wait up to 90s for the cord to stop pulsating naturally, and if the cord does not stop pulsating after 90s, artificial weaning may be more beneficial to maternal and infant outcomes.PMID:38575874 | PMC:PMC10993427 | DOI:10.1186/s12884-024-06444-9… -
A cross-sectional survey of delivery room transitional care management for very/extremely preterm infants in 24 hospitals in Shenzhen City
Zhongguo Dang Dai Er Ke Za Zhi. 2024 Mar 15;26(3):250-257. doi: 10.7499/j.issn.1008-8830.2308017.ABSTRACTOBJECTIVES: To investigate the current status of delivery room transitional care management for very/extremely preterm infants in Shenzhen City.METHODS: A cross-sectional survey was conducted in November 2022, involving 24 tertiary hospitals participating in the Shenzhen Neonatal Data Network. The survey assessed the implementation of transitional care management in the delivery room, including prenatal preparation, delivery room resuscitation, and post-resuscitation management in the neonatal intensive care unit. Very/extremely preterm infants were divided into four groups based on gestational age: <26 weeks, 26-28+6 weeks, 29-30+6 weeks, and 31-31+6 weeks. Descriptive analysis was performed on the results.RESULTS: A total of 140 very/extremely preterm infants were included, with 10 cases in the <26 weeks group, 45 cases in the 26-28+6 weeks group, 49 cases in the 29-30+6 weeks group, and 36 cases in the 31-31+6 weeks group. Among these infants, 99 (70.7%) received prenatal counseling, predominantly provided by obstetricians (79.8%). The main personnel involved in resuscitation during delivery were midwives (96.4%) and neonatal resident physicians (62.1%). Delayed cord clamping was performed in 52 cases (37.1%), with an average delay time of (45±17) seconds. Postnatal radiant warmer was used in 137 cases (97.9%) for thermoregulation. Positive pressure ventilation was required in 110 cases (78.6%), with 67 cases (60.9%) using T-piece resuscitators and 42 cases (38.2%) using a blended oxygen device. Blood oxygen saturation was monitored during resuscitation in 119 cases (85.0%). The median time from initiating transitional care measures to closing the incubator door was 87 minutes.CONCLUSIONS: The implementation of delivery room transitional care management for very/extremely preterm infants in the hospitals participating in the Shenzhen Neonatal Data Network shows varying degrees of deviation from the corresponding expert consensus in China. It is necessary to bridge the gap through continuous quality improvement and multicenter collaboration to improve the quality of the transitional care management and outcomes in very/extremely preterm infants.PMID:38557376 | PMC:PMC10986374 | DOI:10.7499/j.issn.1008-8830.2308017… -
Multicentre, randomised controlled trial of physiological-based cord clamping versus immediate cord clamping in infants with a congenital diaphragmatic hernia (PinC): statistical analysis plan
Trials. 2024 Mar 20;25(1):198. doi: 10.1186/s13063-024-08027-7.ABSTRACTBACKGROUND: Infants born with congenital diaphragmatic hernia (CDH) are at high risk of respiratory insufficiency and pulmonary hypertension. Routine practice includes immediate clamping of the umbilical cord and endotracheal intubation. Experimental animal studies suggest that clamping the umbilical cord guided by physiological changes and after the lungs have been aerated, named physiological-based cord clamping (PBCC), could enhance the fetal-to-neonatal transition in CDH. We describe the statistical analysis plan for the clinical trial evaluating the effects of PBCC versus immediate cord clamping on pulmonary hypertension in infants with CDH (PinC trial).DESIGN: The PinC trial is a multicentre, randomised controlled trial in infants with isolated left-sided CDH, born ≥ 35.0 weeks of gestation. The primary outcome is the incidence of pulmonary hypertension in the first 24 h after birth. Maternal outcomes include estimated maternal blood loss. Neonatal secondary outcomes include mortality before discharge, extracorporeal membrane oxygenation therapy, and number of days of mechanical ventilation. Infants are 1:1 randomised to either PBCC or immediate cord clamping using variable random permutated block sizes (4-8), stratified by treatment centre and estimated severity of pulmonary hypoplasia (i.e. mild/moderate/severe). At least 140 infants are needed to detect a relative reduction in pulmonary hypertension by one third, with 80% power and 0.05 significance level. A chi-square test will be used to evaluate the hypothesis that PBCC decreases the occurrence of pulmonary hypertension. This plan is written and submitted without knowledge of the collected data. The trial has been ethically approved.TRIAL REGISTRATION: ClinicalTrials.gov NCT04373902 (registered April 2020).PMID:38509614 | PMC:PMC10953116 | DOI:10.1186/s13063-024-08027-7… -
Third stage of labor: evidence-based practice for prevention of adverse maternal and neonatal outcomes
Am J Obstet Gynecol. 2024 Mar;230(3S):S1046-S1060.e1. doi: 10.1016/j.ajog.2022.11.1298. Epub 2023 Aug 21.ABSTRACTThe third stage of labor is defined as the time period between delivery of the fetus through delivery of the placenta. During a normal third stage, uterine contractions lead to separation and expulsion of the placenta from the uterus. Postpartum hemorrhage is a relatively common complication of the third stage of labor. Strategies have been studied to mitigate the risk of postpartum hemorrhage, leading to the widespread implementation of active management of the third stage of labor. Initially, active management of the third stage of labor consisted of a bundle of interventions including administration of a uterotonic agent, early cord clamping, controlled cord traction, and external uterine massage. However, the effectiveness of these interventions as a bundle has been questioned, leading to abandonment of some components in recent years. Despite this, upon review of selected international guidelines, we found that the term "active management of the third stage of labor" was still used, but recommendations for and against individual interventions were variable and not necessarily supported by current evidence. In this review, we: (1) examine the physiology of the third stage of labor, (2) present evidence related to interventions that prevent postpartum hemorrhage and promote maternal and neonatal health, (3) review current global guidelines and recommendations for practice, and (4) propose future areas of investigation. The interventions in this review include pharmacologic agents to prevent postpartum hemorrhage, cord clamping, cord milking, cord traction, cord drainage, early skin-to-skin contact, and nipple stimulation. Treatment of complications of the third stage of labor is outside of the scope of this review. We conclude that current evidence supports the use of effective pharmacologic postpartum hemorrhage prophylaxis, delayed cord clamping, early skin-to-skin contact, and controlled cord traction at delivery when feasible. The most effective uterotonic regimens for preventing postpartum hemorrhage after vaginal delivery include oxytocin plus ergometrine; oxytocin plus misoprostol; or carbetocin. After cesarean delivery, carbetocin or oxytocin as a bolus are the most effective regimens. There is inconsistent evidence regarding the use of tranexamic acid in addition to a uterotonic compared with a uterotonic alone for postpartum hemorrhage prevention after all deliveries. Because of differences in patient comorbidities, costs, and availability of resources and staff, decisions to use specific prevention strategies are dependent on patient- and system-level factors. We recommend that the term "active management of the third stage of labor" as a combined intervention no longer be used. Instead, we recommend that "third stage care" be adopted, which promotes the implementation of evidence-based interventions that incorporate practices that are safe and beneficial for both the woman and neonate.PMID:38462248 | DOI:10.1016/j.ajog.2022.11.1298… -
Effect of Placental Transfusion on Long-Term Neurodevelopmental Outcomes in Premature Infants: A Systematic Review and Meta-Analysis of Randomized Controlled Trials
Pediatr Neurol. 2024 May;154:20-25. doi: 10.1016/j.pediatrneurol.2024.01.018. Epub 2024 Feb 1.ABSTRACTBACKGROUND: The pathophysiology and the potential risks of placental transfusion (PT) differ substantially in preterm infants, necessitating specific studies in this population. This study aimed to evaluate the safety and efficacy of PT in preterm infants from the perspective of long-term neurodevelopmental outcomes.METHODS: We conducted a systematic literature search using placental transfusion, preterm infant, and its synonyms as search terms. Cochrane Central Register of Controlled Trials, Medline, and Embase were searched until March 07, 2023. Two reviewers independently identified, extracted relevant randomized controlled trials, and appraised the risk of bias. The extracted studies were included in the meta-analysis of long-term neurodevelopmental clinical outcomes using fixed-effects models.RESULTS: A total of 5612 articles were identified, and seven randomized controlled trials involving 2551 infants were included in our meta-analysis. Compared with immediate cord clamping (ICC), PT may not impact adverse neurodevelopment events. No clear evidence was found of a difference in the risk of neurodevelopmental impairment (risk ratio [RR]: 0.89, 95% confidence interval [CI]: 0.76 to 1.03, P = 0.13, I2 = 0). PT was not associated with the incidence of cerebral palsy (RR: 1.23, 95% CI: 0.59 to 2.57, P = 0.79, I2 = 0). Analyses showed no differences between the two interventions in cognitive, language, and motor domains of neurodevelopment.CONCLUSIONS: From the perspective of long-term neurodevelopment, PT at preterm birth may be as safe as ICC. Future studies should focus on standardized, high-quality clinical trials and individual participant data to optimize cord management strategies for preterm infants after birth.PMID:38452434 | DOI:10.1016/j.pediatrneurol.2024.01.018… -
Impact of the Timing of Umbilical Cord Clamping on Maternal and Neonatal Outcomes in Saudi Arabia
Cureus. 2024 Feb 4;16(2):e53536. doi: 10.7759/cureus.53536. eCollection 2024 Feb.ABSTRACTINTRODUCTION: The optimal time for umbilical cord clamping after delivery has been under debate for several decades. This study aimed to assess the time-dependent effects of umbilical cord clamping on maternal and neonatal outcomes.METHODS: An observational correlational design was used to recruit 161 pregnant women conveniently. Outcomes were observed and recorded using a structured checklist developed by the authors. Pregnant females aged ≥18 years, with uncomplicated delivery, and who were willing to participate were recruited. Exclusion criteria included stillbirths, newborns with congenital anomalies, newborns too small for their gestational age, intra-uterine growth restriction, nuchal cord, and meconium-stained liquor.RESULTS: The mean age of the participants was 29.93 ± 6 years. Early clamping (<1 minute) was performed for 93.8% of the participants with a mean of 29.58 ± 18 seconds. Delayed clamping was associated with a decrease in blood loss and the length of hospital stay in addition to an increase in first-minute APGAR score and neonatal temperature (P < 0.05).CONCLUSIONS: Delayed cord clamping was associated with improved maternal and neonatal outcomes.PMID:38445130 | PMC:PMC10912892 | DOI:10.7759/cureus.53536… -
Physiological-based cord clamping in very preterm infants: the Aeration, Breathing, Clamping 3 (ABC3) trial-statistical analysis plan for a multicenter randomized controlled trial
Trials. 2024 Mar 4;25(1):164. doi: 10.1186/s13063-024-08014-y.ABSTRACTBACKGROUND: Mortality, cerebral injury, and necrotizing enterocolitis (NEC) are common complications of very preterm birth. An important risk factor for these complications is hemodynamic instability. Pre-clinical studies suggest that the timing of umbilical cord clamping affects hemodynamic stability during transition. Standard care is time-based cord clamping (TBCC), with clamping irrespective of lung aeration. It is unknown whether delaying cord clamping until lung aeration and ventilation have been established (physiological-based cord clamping, PBCC) is more beneficial. This document describes the statistical analyses for the ABC3 trial, which aims to assess the efficacy and safety of PBCC, compared to TBCC.METHODS: The ABC3 trial is a multicenter, randomized trial investigating PBCC (intervention) versus TBCC (control) in very preterm infants. The trial is ethically approved. Preterm infants born before 30 weeks of gestation are randomized after parental informed consent. The primary outcome is intact survival, defined as the composite of survival without major cerebral injury and/or NEC. Secondary short-term outcomes are co-morbidities and adverse events assessed during NICU admission, parental reported outcomes, and long-term neurodevelopmental outcomes assessed at a corrected age of 2 years. To test the hypothesis that PBCC increases intact survival, a logistic regression model will be estimated using generalized estimating equations (accounting for correlation between siblings and observations in the same center) with treatment and gestational age as predictors. This plan is written and submitted without knowledge of the data.DISCUSSION: The findings of this trial will provide evidence for future clinical guidelines on optimal cord clamping management at birth.TRIAL REGISTRATION: ClinicalTrials.gov NCT03808051. Registered on 17 January 2019.PMID:38439024 | PMC:PMC10913647 | DOI:10.1186/s13063-024-08014-y…
ALtimetric score
Measure of how our paper in JAMA Pediatrics 2017 on anemia is spread by media
Measure of how our paper in JAMA Pediatrics 2015 on neurodevelopment is spread by media